Abilify
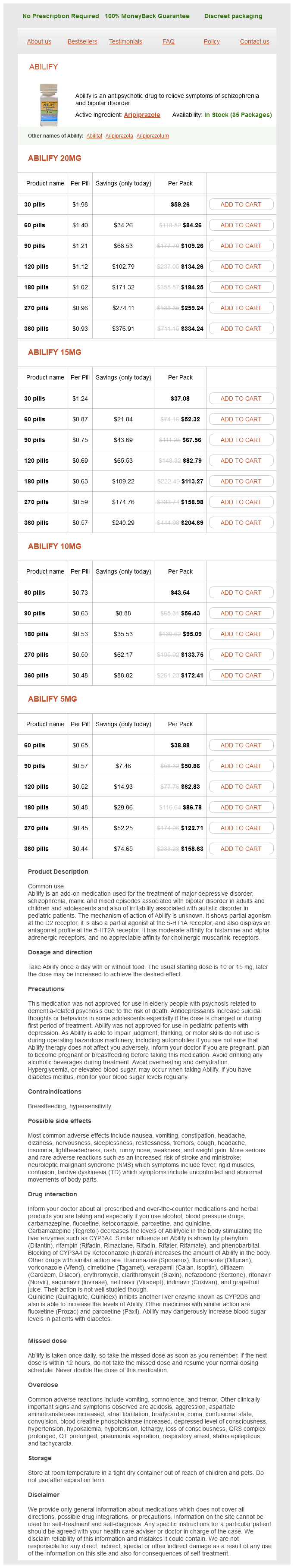
Abilify Dosage and Price
Abilify 20mg
- 30 pills - $59.26
- 60 pills - $84.26
- 90 pills - $109.26
- 120 pills - $134.26
- 180 pills - $184.25
- 270 pills - $259.24
- 360 pills - $334.24
Abilify 15mg
- 30 pills - $37.08
- 60 pills - $52.32
- 90 pills - $67.56
- 120 pills - $82.79
- 180 pills - $113.27
- 270 pills - $158.98
- 360 pills - $204.69
Abilify 10mg
- 60 pills - $43.54
- 90 pills - $56.43
- 180 pills - $95.09
- 270 pills - $133.75
- 360 pills - $172.41
Abilify 5mg
- 60 pills - $38.88
- 90 pills - $50.86
- 120 pills - $62.83
- 180 pills - $86.78
- 270 pills - $122.71
- 360 pills - $158.63
Nocardiosis in liver transplantation: Variation in presentation 8 dpo anxiety order abilify 10 mg mastercard, diagnosis and therapy. Disseminated Nocardia transvalensis infection resembling pulmonary infarction in a liver transplant recipient. Lung abscess complicating Legionella micdadei pneumonia in an adult liver transplant recipient: Case report and review. Infection with Listeria monocytogenes following orthotopic liver transplantation: Case report and review of the literature. Risk factors for postoperative respiratory complications in adult liver transplant recipients. Piperacillintazobactam versus ciprofloxacin plus amoxicillin in the treatment of infective episodes after liver transplantation. Efficacy of galactomannan antigen in the Platelia Aspergillus enzyme immunoassay for diagnosis of invasive aspergillosis in liver transplant recipients. Asymptomatic pulmonary cryptococcosis in solid organ transplantation: Report of four cases and review of the literature. Clinical spectrum of invasive cryptococcosis in liver transplant recipients receiving tacrolimus. Cryptococcal meningitis: An analysis among 5,521 consecutive organ transplant recipients. Invasive gastrointestinal zygomycosis in a liver transplant recipient: Case report and review of zygomycosis in solid-organ transplant recipients. Zygomycosis in solid organ transplant recipients in a tertiary transplant center and review of the literature. Infection in solid organ transplant recipients in a tertiary medical center and review of the literature. Combination therapeutic approaches for the management of invasive aspergillosis in organ transplant recipients. Randomized trial of fluconazole versus nystatin for the prophylaxis of Candida infection following liver transplantation. Fluconazole prophylaxis of fungal infections in liver transplant recipients: Results of a placebo-controlled, double blind trial. Prophylactic fluconazole in liver transplant recipients: A randomized, double-blind, placebo-controlled trial. Randomized controlled trial of oral itraconazole solution versus intravenous/oral fluconazole for prevention of fungal infections in liver transplant recipients. Efficacy and safety of itraconazole prophylaxis for fungal infections after orthotopic liver transplantation: A prospective, randomized, double-blind study. Liposomal amphotericin B prevents invasive fungal infections in liver transplant recipients. Randomized, doubleblind trial of fluconazole versus voriconazole for prevention of invasive fungal infection after allogeneic hematopoietic cell transplantation. Trends in invasive fungal infections in liver transplant recipients: Correlation with evolution in transplant practices. Association of fungal infection and increased mortality in liver transplant recipients. Changes in the spectrum and risk factors for invasive candidiasis in liver transplant recipients: Prospective, multicenter, case-controlled study. Surveillance and treatment of liver transplant recipients for candidiasis and aspergillosis. Risk factors of invasive candida and non-candida fungal infections after liver transplantation. Candida krusei: Biology, epidemiology, pathogenicity and clinical manifestations of an emerging pathogen. Selection of Candida glabrata with reduced susceptibility to azoles in four liver transplant recipients with invasive candidiasis. Factors associated with the development of candidemia and candidemia-related death among liver transplant recipients. Incidence and significance of Aspergillus cultures following liver and kidney transplantation. Trends in risk profiles for and mortality associated with invasive aspergillosis among liver transplant recipients. Opportunistic mycelial fungal infections in organ transplant recipients: Emerging importance of non-Aspergillus mycelial fungi. Cryptococcus neoformans infection in organ transplant recipients: Variables influencing clinical characteristics and outcome. Pseudallescheria boydii endocarditis of the pulmonic valve in a liver transplant recipient. Factors associated with invasive lung aspergillosis and the significance of positive Aspergillus culture after liver transplantation. Micafungin: a review of its use in the prophylaxis and treatment of invasive candida infections. Micafungin versus fluconazole for prophylaxis against invasive fungal infections during neutropenia in patients undergoing hematopoietic stem cell transplantation. Prophylaxis with caspofungin for invasive fungal infections in high risk liver transplant recipients. Preemptive prophylaxis with a lipid preparation of amphotericin B for invasive fungal infections in liver transplant recipients requiring renal replacement therapy. Fungal infection and liposomal amphotericin B (AmBisome) therapy in liver transplantation: A 2 year review. Systemic mycoses during prophylactical use of liposomal amphotericin B (Ambisome) after liver transplantation.
Mammalian target of rapamycin inhibitors should be considered as a rescue therapy in those refractory to antimetabolites depression symptoms mild cheap abilify online american express. Those advances need to be accompanied by clinicians willing to research and study the optimal way to utilize these medications, and these clinicians and companies need to be supported by regulatory and governmental bodies that recognize how the goals of modern immunosuppression have changed over 35 years. With all three of these aims in place, immunosuppression will continue to advance the field of liver transplantation. Immunosuppressive agents in solid organ transplantation: Mechanisms of action and therapeutic activity. Bioavailability and pharmacokinetics of cyclosporine formulations: Neoral vs Sandimmune. Clinical pharmacokinetics and pharmacodynamics of tacrolimus in solid organ transplantation. Tacrolimus trough levels, rejection and renal impairment in liver transplantation: a systematic review and meta-analysis. Changing picture of center of central nervous system complications in liver transplant recipients. Effects of the new and highly active immunosuppressant rapamycin on lymphoid tissues and cells in vivo. Sirolimus steady-state trough concentrations are not affected by bolus methylprednisolone therapy in renal allograft recipients. Mammalian target of rapamycin positively regulates collagen type 1 production via a phosphatidylinositol 3-kinase-independent pathway. Rapamycin inhibits spontaneous and fibroblast growth factor beta-stimulated proliferation of endothelial cells and fibroblasts. Rapamycin ameliorates proteinuria-associated tubulointerstitial inflammation and fibrosis in experimental membranous nephropathy. Risk factors for impaired wound healing in sirolimus-treated renal transplant recipients. Incisional hernia following liver transplantation: incidence and predisposing factors. Sirolimus-associated interstitial pneumonitis in solid organ transplant recipients. A retrospective review of liver transplant patients treated with sirolimus from a single center: an analysis of sirolimus-related complications. Multicentric outcome analysis of sirolimus-based immunosuppression in 252 liver transplant recipients. Pharmacokinetics of the immunosuppressant everolimus in maintenance renal transplant patients. A comprehensive review of everolimus clinical reports: a new mammalian target of rapamycin inhibitor. Structure and mechanism of inosine monophosphate dehydrogenase in complex with the immunosuppressant mycophenolic acid. Mycophenolate mofetil: Effects on cellular immune subset, infectious complications and antimicrobial activity. Pharmacokinetics and bioavailability of mycophenolate mofetil in heathy subjects after single-dose oral and intravenous administration. Clinical pharmacokinetics and pharmacodynamics of mycophenolate in solid organ transplant recipients. Reviewing the mechanism of action of thiopurine drugs: Towards a new paradigm in clinical practice. Myelosuppression associated with azathioprine-allopurinol interaction after heart and lung transplantation. Interaction of ribavirin with azathioprine metabolism potentially induces myelosuppression. The use of heterologous antilymphoid agents in canine renal and liver homotransplantation and in human renal homotransplantations. A comprehensive definition of the major antibody specification in polyclonal rabbit antithymocyte globulin. Serum sickness following rabbit antithymocyte globulin induction in a liver transplant recipient: Case report and literature review. Serum sickness after treatment with rabbit antithymocyte globulin in kidney transplant recipients with previous rabbit exposure. Sotrastaurin, a novel small molecule inhibiting protein kinase C: First clinical results in renal-transplant recipients. Alefacept combined with tacrolimus, mycophenolate mofetil and steroids in de novo kidney transplantation: a randomized controlled trial. Outcome of induction immunosuppression for liver transplantation comparing antithymocyte globulin, daclizumab, and corticosteroid. Anti-Interleukin-2 receptor therapy in combination with mycophenolate mofetil is associated with more severe hepatitis C recurrence after liver transplantation. Preserving renal function in liver transplant recipients with rabbit anti-thymocyte globulin and delayed initiation of calcineurin inhibitors. Steroid-free liver transplantation using rabbit anti-thymocyte globulin and early tacrolimus monotherapy. Evaluation of renal function in liver transplant recipients receiving daclizumab (Zenapax), mycophenolate mofetil, and a delayed low-dose tacrolimus regimen vs a standard-dose tacrolimus and mycophenolate mofetil regimen: a multicenter randomized clinical trial. Assessing renal function with daclizumab induction and delayed tacrolimus introduction in liver transplant recipients. Corticosteroid-free immunosuppression with tacrolimus following induction with daclizumab: a large randomized clinical study.
Intermittent celiac trunk stenosis may be caused by the arcuate ligament impairing patency of the trunk during inspiration; a persistent stenosis may be congenital or related to arteriosclerosis depression chinese definition generic abilify 20 mg amex. In the latter case an arterial jump graft is advised, and intermittent stenosis can be avoided by incision of the arcuate ligament. Further technical reasons may be related to the delicate vascular supply of the bile duct. The same applied to organs harvested externally versus those procured locally (P <. However, despite the description of distinct histological findings of extrahepatic cholestasis resulting from extrahepatic obstruction, the liver biopsy can miss an extrahepatic obstruction by misinterpreting portal inflammation as rejection,87 thus confusing the primary diagnosis and leading to the misdiagnosis of rejection. Imaging the subsequently shown diagnostic workup has been reviewed repeatedly in an attempt to reach the most accurate strategy. Complaints such as right upper quadrant abdominal pain, anorexia, abdominal distention, singultus, paralytic ileus, and right shoulder pain are typically associated with biliary tract disorders but are not specific or could be absent. Pain, a leading concern, can be totally absent in liver transplant patients due to hepatic denervation. Fever may accompany biliary leakage or cholangitis but is usually indicative for infections of various kinds. Bile leaks should also be considered in asymptomatic patients with unexplained elevations in serum bilirubin level, unexplained fluctuations in cyclosporine levels, bilious ascites, or intraperitoneal fluid collections on imaging studies. In contrast, Hussaini et al96 reported an overall sensitivity of 77% and a specificity of 67%, with positive and negative predictive values of 26% and 95%, respectively, when adjusted to an endoscopically assessed complication rate of 12. Commonly a transient increase in the levels of liver enzymes 1 to 2 days following T-tube clamping will occur. Conversely, liver biopsy results were usually abnormal in this subset of patients and should therefore be the initial invasive procedure. Specific combinations of contrast medium provide negative gastrointestinal contrast on both T1- and T2-weighted sequences without causing significant susceptibility artifacts. However, formal comparative studies with other imaging modalities have not yet been published. The sensitivity and specificity were more than 90%, and the positive predictive value was reported to be 86%. Also, proximal biliary dilatation may be absent despite significant stenosis at the anastomotic site. However, its value in screening for biliary obstruction or leaks still awaits evaluation in imaging studies. Proper care of the graft before transplantation and accurate surgical technique are important features to avoid posttransplant biliary complications. The prompt recognition and management of these complications ensures complete and definitive treatment in many cases. Leaks occur preferentially in the early posttransplant period (within 1 month of surgery). Stricture formation typically develops gradually over several months to years, depending on the degree of the insult. The annual incidence of biliary complications was reported to be less than 4% after the first posttransplant year. However, the incidence of biliary problems is highest in the first few months after transplantation. It declines to very low incidences after the first posttransplantation year, but occasionally biliary problems appear after several years. Anastomotic leaks are caused primarily by ischemic necrosis at the end of the bile duct (most commonly the donor duct) or a technically unsatisfactory anastomosis. Nonanastomotic, nonÂT-tube-related leaks often result from vascular insufficiency. Endoscopic retrograde cholangiography displayed a broad anastomotic leakage resulting in a release of radiopaque contrast into the subhepatic space. Bile leakage from any source can be serious; however, leaks from the anastomosis are the most hazardous. Anastomotic leaks can be visualized with a T-tube cholangiogram and managed conservatively by leaving the T tube open to divert bile flow. A repeat cholangiogram in 1 to 2 weeks eventually confirms healing of the bile duct. The involvement of the intestinal loop presumably contributes to an increased chance of intra-abdominal abscess formation and sepsis. Bile leaks may complicate up to 33% of all T-tube removals, depending on the diagnostic criteria used. There is no clear correlation between either progressive duct dilation or graft ischemia time and the subsequent development of bile leak after T-tube removal. An impact of T-tube removal earlier than the usual period of 6 weeks to 3 months has not yet been confirmed. The presentation is usually a combination of massive bile leakage, sepsis, cholestasis, and associated complications such as pleural effusion. They are sometimes caused by recurrence or persistence of early complications or can be due to delayed removal of T tubes, transhepatic anastomotic stents, or biliary stent migration and perforation. Despite recurrent cholangitis and cholestasis secondary to ischemic injury of the biliary tree, synthetic graft function may still be good. Hence nondefinitive, temporary measures may often be considered until definitive treatment by retransplantation is necessary. One of the most feared secondary complications is massive and often deleterious erosion bleeding of the hepatic artery.